Uveitis is not just a red eye. It’s a serious inflammation deep inside the eye that can steal your vision-sometimes without warning. If you’ve noticed sudden eye pain, blurry vision, or floaters that won’t go away, this isn’t something to brush off. Uveitis affects the uvea, the middle layer of your eye that includes the iris, ciliary body, and choroid. This layer feeds blood to key parts of your eye, and when it swells, it doesn’t just hurt-it can damage your retina, lens, or optic nerve. Left untreated, uveitis becomes one of the top three causes of blindness worldwide.
What Exactly Is the Uvea?
The uvea isn’t one single part. It’s three layers stacked together. The front part, the iris, controls how much light enters your eye. Behind it is the ciliary body, which helps focus your lens and makes the fluid inside your eye. The back part, the choroid, is packed with blood vessels that feed the retina. When inflammation hits any of these, it’s uveitis. The location of the inflammation determines the type, symptoms, and how it’s treated.The Four Types of Uveitis
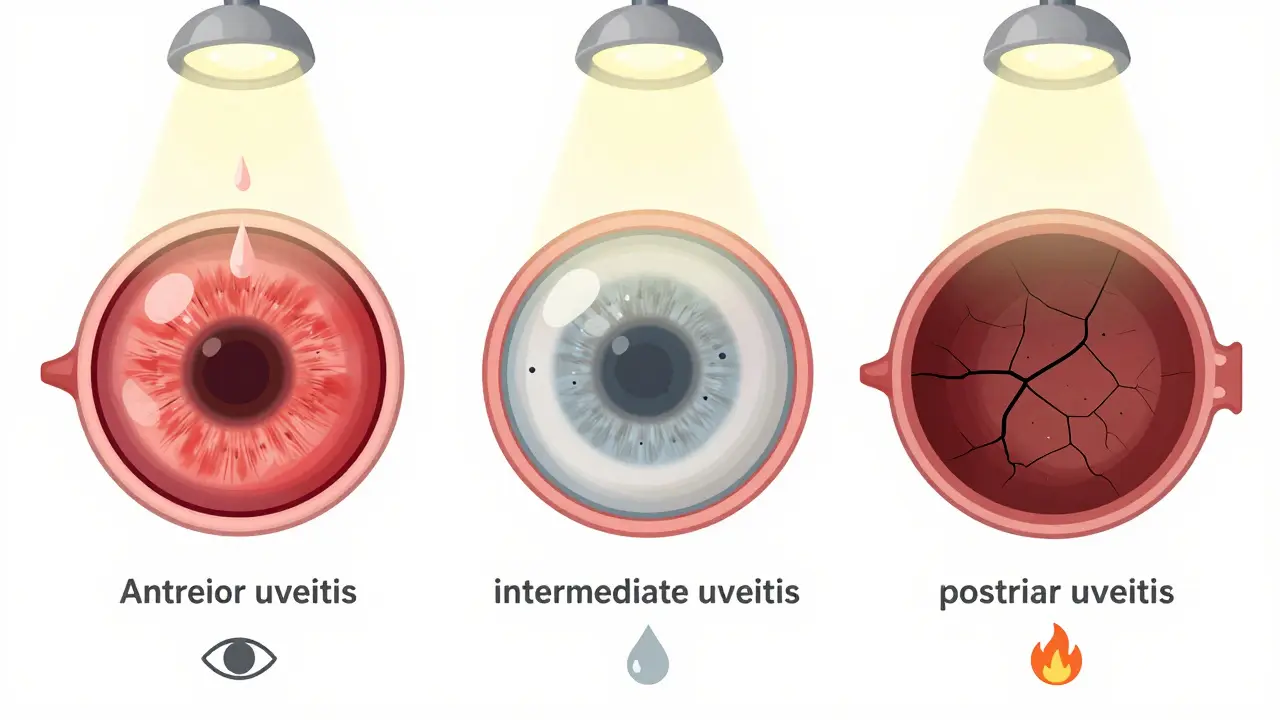
Not all uveitis is the same. Doctors classify it by where the swelling happens:- Anterior uveitis (iritis) is the most common-making up 75% to 90% of cases. It hits the front, near the iris. Symptoms show up fast: red eye, sharp pain, light sensitivity, and blurred vision. You might notice it when reading, because focusing strains the inflamed iris. This type usually responds well to eye drops.
- Intermediate uveitis (pars planitis) affects the vitreous, the jelly-like fluid in the center of the eye. It’s less painful but causes floaters-those dark spots or squiggles drifting across your vision-and blurry sight. It often lasts longer, sometimes years, and can lead to swelling in the macula, the part of the retina that gives you sharp central vision.
- Posterior uveitis attacks the choroid and retina at the back of the eye. This is the most dangerous form. It often affects both eyes and develops slowly, so you might not notice until your vision is already fading. It’s the main cause of permanent vision loss in uveitis patients.
- Panuveitis means all layers are inflamed. It combines symptoms from all the others: pain, floaters, blurred vision, and severe swelling. It’s rare but the most serious.
Acute uveitis lasts less than six weeks. Chronic uveitis sticks around longer and can flare up again and again. The longer inflammation goes untreated, the more damage it does to your eye’s structure.
What Causes Uveitis?
Here’s the tricky part: doctors can’t find a clear cause in about one-third of cases. That’s called idiopathic uveitis. But when they can, the triggers fall into three big groups.- Autoimmune diseases: Your immune system attacks your own eye tissue. Conditions like ankylosing spondylitis, sarcoidosis, multiple sclerosis, and rheumatoid arthritis are common culprits. If you have one of these, your eye inflammation might be a sign your body is out of balance.
- Infections: Viruses like herpes simplex or shingles (herpes zoster), bacteria like syphilis, or parasites like toxoplasmosis can spread to the eye. Even fungal infections like histoplasmosis-common in certain parts of the U.S.-can trigger uveitis.
- Eye trauma or surgery: A scratch, a blow to the eye, or even recent eye surgery can spark inflammation. Sometimes, the body overreacts to the injury.
It’s not just about what’s in your eye. Uveitis is often a signal that something deeper is going on in your body. That’s why your eye doctor might send you to a rheumatologist or infectious disease specialist.
Steroid Therapy: The First-Line Treatment
Steroids are the backbone of uveitis treatment. They work fast to calm inflammation and prevent permanent damage. But how you get them depends on where the inflammation lives.- Anterior uveitis: Steroid eye drops-like prednisolone acetate 1%-are the go-to. You’ll start with drops every hour or two, then taper down over weeks as the swelling fades. Sometimes, a dilating drop is added to keep the iris from sticking to the lens.
- Intermediate uveitis: Eye drops don’t reach far enough. Doctors often use injections around the eye (periocular) or implant tiny steroid devices inside the eye (intravitreal). Oral steroids may be needed if it’s severe or recurrent.
- Posterior uveitis: This needs strong, systemic treatment. Oral prednisone is common, sometimes with other immunosuppressants. Injections or implants are used if the inflammation is focused on the retina.
- Panuveitis: Usually requires oral steroids plus close monitoring. Some patients need long-term immunosuppressants to avoid constant steroid use.
Timing matters. The sooner you start steroids after symptoms appear, the better your chances of saving your vision. Delaying treatment even a few days can mean irreversible damage to your retina or optic nerve.
The Dark Side of Steroids
Steroids work-but they come with risks. Long-term use can cause cataracts, where your lens clouds over. It can also raise pressure inside your eye, leading to steroid-induced glaucoma. About 30-40% of people on long-term oral steroids develop one or both of these problems.This is why doctors don’t just give steroids and walk away. They monitor eye pressure every few weeks. They check for cataracts with regular scans. And if uveitis keeps coming back, they switch to steroid-sparing drugs-medicines like methotrexate, mycophenolate, or anti-TNF biologics-that control inflammation without the side effects. These take longer to work, but they’re safer for the long haul.
When to See a Doctor
If you have any of these symptoms, don’t wait:- Sudden red eye with pain
- Blurred vision that doesn’t clear up
- Floaters that multiply or get worse
- Extreme sensitivity to light
- Vision loss in one or both eyes
Uveitis is not like a cold. It doesn’t go away on its own. Even if symptoms fade, the inflammation might still be there, quietly damaging your eye. A routine eye exam can catch posterior uveitis before you even notice a problem.
What Happens If It’s Not Treated?
Untreated uveitis doesn’t just cause blurry vision. It leads to:- Macular edema: Fluid builds up in the central retina, blurring your ability to read or recognize faces.
- Synechiae: The iris sticks to the lens or cornea, changing your pupil shape and blocking fluid flow-this can raise eye pressure and cause glaucoma.
- Cataracts: Clouding of the lens from chronic inflammation or steroid use.
- Glaucoma: High pressure inside the eye damages the optic nerve.
- Retinal detachment: Inflammation weakens the retina, causing it to peel away.
- Permanent vision loss: Especially in posterior uveitis and panuveitis.
Once this damage happens, it’s often irreversible. That’s why uveitis is treated like an emergency-even if the pain fades.
Living With Chronic Uveitis
If your uveitis is chronic, you’ll need ongoing care. Regular eye exams every 3-6 months are standard. You might need blood tests to check for underlying autoimmune disease. Some patients learn to recognize early signs of a flare-like a slight increase in floaters-and call their doctor before symptoms get bad.Managing stress, quitting smoking, and keeping other health conditions (like high blood pressure or diabetes) under control can help reduce flare-ups. There’s no cure, but with the right treatment plan, most people keep good vision for life.
Can uveitis go away on its own?
No. Even if symptoms like pain or redness disappear, inflammation inside the eye can still be active and damaging your retina or optic nerve. That’s why treatment is always needed-even if you feel better.
Is uveitis contagious?
No. Uveitis itself isn’t contagious. But if it’s caused by an infection like herpes or syphilis, those underlying infections can be spread to others. The eye inflammation is your body’s reaction-not something you can catch from someone else.
Can I use over-the-counter eye drops for uveitis?
Absolutely not. OTC redness-relief drops won’t touch the deep inflammation. They might even mask symptoms, delaying diagnosis. Only prescription steroid eye drops, under a doctor’s supervision, can safely treat uveitis.
Do steroids cure uveitis?
Steroids don’t cure it-they control it. They stop the inflammation so your eye can heal. But if the root cause (like an autoimmune disease) isn’t addressed, uveitis can come back. That’s why long-term management often includes other immune-modifying drugs.
Can uveitis affect both eyes?
Yes. Anterior uveitis usually starts in one eye, but it can spread to the other. Intermediate, posterior, and panuveitis often affect both eyes from the start. That’s why doctors check both eyes during exams-even if only one feels bad.


Jacob Carthy
February 25, 2026 AT 23:33Joanna Reyes
February 26, 2026 AT 07:10Joseph Cantu
February 26, 2026 AT 10:15Spenser Bickett
February 27, 2026 AT 22:16Nerina Devi
February 28, 2026 AT 10:44Gabrielle Conroy
February 28, 2026 AT 22:40Stephen Archbold
March 2, 2026 AT 17:18Cory L
March 3, 2026 AT 04:30Anil bhardwaj
March 3, 2026 AT 17:20Haley Gumm
March 5, 2026 AT 01:52Dinesh Dawn
March 6, 2026 AT 00:41Lisandra Lautert
March 7, 2026 AT 07:02