Why Small Measurement Errors Matter Big
When you pour liquid medicine, you might think a teaspoon is close enough. It isn't. Studies show that nearly half of caregivers make mistakes significant enough to cause harm when measuring liquids. In fact, error rates range between 15% and 43% depending on which tool you grab off the shelf. These aren't minor slips; they are clinically significant deviations where patients receive too little or way too much medicine. For children especially, incorrect dosing leads to roughly 30% of all medication emergencies.
Dosing devices are tools designed to measure precise volumes of liquid medication for safe administration. They include oral syringes, graduated cups, and specialized spoons. When you use the wrong tool, you risk under-dosing or overdosing your patient. The gap between "close" and "accurate" is often the difference between recovery and hospitalization. In 2025, new regulations mandated that all new liquid approvals must include metric-only labeling and scaled devices. If you are holding a bottle today, checking these tools is the first line of defense for safety.
Picking the Right Tool for the Job
You have options, but not all options work equally well. Many people default to the plastic cup that came inside the box because it feels familiar. However, that familiarity often hides poor visibility. Oral syringes consistently outperform other tools in tests. A study found that for a 2.5 mL dose, syringes had only a 4% error rate. That same task performed with a 30-mL cup resulted in a 43% error rate. The difference is massive.
| Device Type | Typical Error Rate | Best Use Case |
|---|---|---|
| Oral Syringe | 4% | Volumes under 5 mL |
| Dosing Spoon | 4.5% | Small doses, easy pouring |
| Graduated Cup | 14.6% to 43% | Larger volumes over 10 mL |
| Household Spoon | Up to 80% | Avoid completely |
Spoons perform better than cups but still struggle compared to syringes. Household spoons are the biggest hazard. A standard kitchen teaspoon holds different amounts of liquid every time you scoop. One time you might get 4 mL, the next 6 mL. Experts state that using household spoons is responsible for approximately 40% of liquid medication errors in children. Always discard the kitchen spoon if the pharmacy hasn't provided a calibrated alternative. If you are treating adults who need larger doses, a properly marked cup works better, provided it doesn't have confusing extra markings.
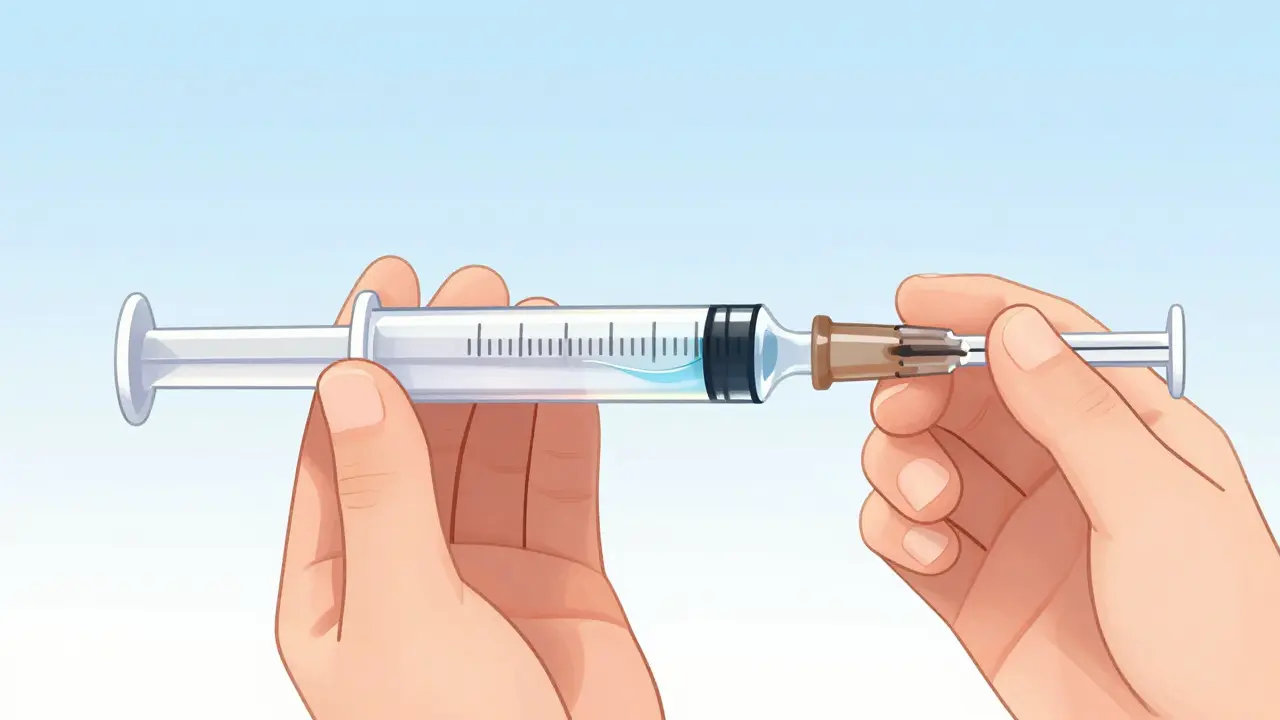
Understanding the Markings on Your Device
Most mistakes happen before you even touch the liquid. You look at the bottle label and try to match it with the device. If the label says "teaspoon" but the device measures "milliliters," you are setting yourself up for failure. Regulatory bodies like the FDA have pushed for years to standardize everything to milliliters. By 2025, enforcement increased significantly to require metric units exclusively on new approvals.
You need to spot specific design flaws immediately. Look for leading zeros. The number 0.5 mL is safer than .5 mL. If you miss that dot, you give ten times the dose. Similarly, watch for trailing zeros. "5 mL" is correct; "5.0 mL" invites confusion about precision. If a device shows both teaspoons and milliliters, ignore the teaspoon side. Using two systems increases cognitive load and raises the chance of misreading. Standardizing exclusively on milliliters reduces brain fog during stressful moments when a child is sick.
Liquid Medications are pharmaceutical formulations dissolved or suspended in fluid requiring volume-based measurement. Their accuracy depends entirely on the delivery device used.Check the container label against the device graduations. Ideally, the increments on your syringe or cup should match the prescribed dose. If your child needs 3.75 mL, a syringe with marks every 1 mL is useless. You need one with 0.25 mL markings. A study showed that 81% of devices included superfluous markings that didn't match the prescription. If the cup goes up to 30 mL but you only ever take 2 mL, you cannot measure precisely. Ask your pharmacist for a device sized specifically for that dose.
Mastery of Measurement Technique
Having the right tool is only half the battle. You must handle it correctly. Parallax error occurs when you view the measurement from an angle rather than straight on. Imagine looking at a ruler through water; the lines shift slightly. When measuring medicine, hold the device at eye level. If you look down into a cup, the liquid looks higher than it is. If you look up at a syringe, it reads low. Both lead to dosing errors.
- Draw air into the syringe tip first. This clears the needleless tip so the liquid enters immediately.
- Insert the tip below the surface of the liquid. Pull back slowly.
- Tap the syringe gently to move any trapped bubbles to the top.
- Align your eyes with the measurement mark on the barrel.
- Read the bottom of the meniscus curve where the liquid meets the glass or plastic.
The meniscus is the curved surface of the liquid caused by tension. It always dips slightly in the center. You must measure to the bottom of that dip, not the sides touching the container. This tiny distinction can add up to 10% variation in volume. The United States Pharmacopeia established a standard that volume error should not exceed 10% of the indicated amount. To stay within this safety window, steady hands and clear sightlines are non-negotiable.
Bubbles are another silent enemy. Trapped air takes up space meant for the medication. If you see a bubble in the barrel above the line, you haven't drawn enough medicine. Tap the side of the syringe to pop them and push them back up into the vial. Never force the liquid into the vial to remove bubbles after drawing the full dose, as you might lose pressure and drop the volume below the target line.

Matching Labels to Devices in Real Time
Consistency is the ultimate safety goal. The instruction on the prescription container must exactly match the markings on the device. Inconsistent labeling accounts for roughly 20% of all liquid medication errors. If the label says "5 ml" but the cup only has marks for "10 ml" and "15 ml", you cannot estimate the middle safely. You need marks that correspond directly to your dose.
Many modern pharmacies now offer QR codes on labels. Scanning these links to videos showing exactly how to use the specific device provided with that bottle. This practice, implemented by major chains by early 2026, helps bridge the gap between professional instruction and home care. If you don't have a QR code, ask the pharmacist to demonstrate. The "teach-back" method works wonders. Show them how you plan to draw the dose, then have them confirm it back to you.
Document quality plays a huge role here. Only about 41% of labels previously included proper dosing instructions clearly. Facilities using standardized templates improved compliance to 92%. If your label is handwritten or ambiguous, request a reprint. Do not guess. If the unit of measure isn't clear, clarify before leaving the counter. Ambiguity is where risk hides.
Troubleshooting Common User Friction Points
People resist syringes for good reasons. Some feel like needles. Others find drawing liquid messy. Resistance peaks at 58% among pediatric nurses regarding caregiver comfort levels. Despite this preference, safety dictates accuracy over convenience. If a parent refuses a syringe because it looks scary, try a different design. There are syringes with blunt tips specifically made for oral use that prevent accidental piercing.
If spills are frequent, check your grip. Holding the plunger loosely allows it to slip. Hold the barrel firmly near the tip, not just at the back. Practice makes muscle memory. Spend five minutes with water before doing it for real. Water costs nothing; an overdose costs health. Also, consider the lighting. Poor light obscures the meniscus. Turn on the brightest lamp in the room. Shadows hide volume discrepancies.
Economic disparities often mean lower-quality devices reach vulnerable patients. Some studies suggest low-income patients receive less accurate tools 63% of the time. Check your device quality manually. High-quality plastic doesn't stain easily, and markings are laser-etched rather than stamped ink that washes off. If your device degrades quickly, replace it. Don't reuse disposable syringes beyond the recommended period as markings may fade or material may warp.

Owen Barnes
April 2, 2026 AT 07:59tis really interesting how many people still use kitchen spoons insted of proper tools i think its sad that we dont teach this in schools yet we risk health daily
Cullen Zelenka
April 2, 2026 AT 11:20i hope this helps everyone stay safe and happy during sick seasons we can do better together
Christopher Beeson
April 4, 2026 AT 09:40society crumbles when the smallest details are ignored and we see the fragility of life in these statistics it is terrifying how much negligence hides in plain sight
Sharon Munger
April 4, 2026 AT 18:21syringes are way better than cups.
Rod Farren
April 5, 2026 AT 00:32youre missing the nuance of the meniscus effect on volumetric accuracy the calibration tolerance is critical here
Eleanor Black
April 5, 2026 AT 16:58I truly believe that understanding the gravity of measurement errors is essential for every caregiver who touches medicine. We must consider the child sitting on the edge of recovery and waiting for help. The difference between health and harm lies in our hands during those quiet moments at home. Every mark on the plastic barrel represents a promise of safety that we cannot ignore lightly. If we choose the wrong tool we inadvertently place trust in a flawed process rather than science. The studies mentioned indicate that familiarity breeds complacency which leads to dangerous assumptions about volume. It is vital to remember that household cutlery is manufactured for food not pharmaceutical solutions. We must educate ourselves to demand proper devices from pharmacies regardless of comfort or habit. A small investment in the right syringe prevents a trip to the emergency room which costs far more emotionally. When we standardize metrics we remove the confusion that clouds judgment during stressful illness events. This collective effort builds a stronger foundation for public health outcomes everywhere we live. Let us commit to checking every label against every device before administering a single drop. The peace of mind gained from accuracy outweighs any minor inconvenience of setup time. Families deserve the best chance at healing without the shadow of preventable mistakes hanging over them. We owe it to our loved ones to master this skill of precise dosage management today.
James DeZego
April 7, 2026 AT 10:40great tips on the QR codes those videos make it so easy to follow along 🙂
Jenny Gardner
April 7, 2026 AT 13:21This discussion highlights the severity of the situation! Indeed, precision matters! The data supports your argument well! One must never underestimate the risk!
Arun Kumar
April 7, 2026 AT 19:41i see how different countries handle this differently but metric is definitely the universal language we need now
Rocky Pabillore
April 8, 2026 AT 02:59most people lack the intellect to grasp basic measurement concepts without constant hand holding from professionals
Julian Soro
April 9, 2026 AT 08:27we can all learn and improve with practice so let us focus on getting the right tools for everyone
Cara Duncan
April 9, 2026 AT 18:55love seeing people share knowledge 🙏 lets keep supporting each other 🌟
Russel Sarong
April 11, 2026 AT 11:54How did you figure that out?! Why didn t anyone tell us sooner?? We need more awareness!!! Is there a campaign running??? Please share everything you know!!!
Callie Bartley
April 13, 2026 AT 01:58another useless thread nobody reads past the title and we waste time arguing